Prioritising Healthcare for a Viksit Bharat 2047
Budget 2026–27 and India’s Expanding Public Health Vision
S Ahmad
As India advances toward its long-term goal of becoming a Viksit Bharat by 2047, healthcare has moved from being a welfare obligation to becoming a central pillar of national development strategy. The Union Budget 2026–27 reflects this shift with clarity and conviction. At a time when the country faces complex health transitions—from infectious diseases to lifestyle disorders, from undernutrition to ageing demographics—the government has chosen to respond with increased allocations, systemic reforms, and forward-looking investments.
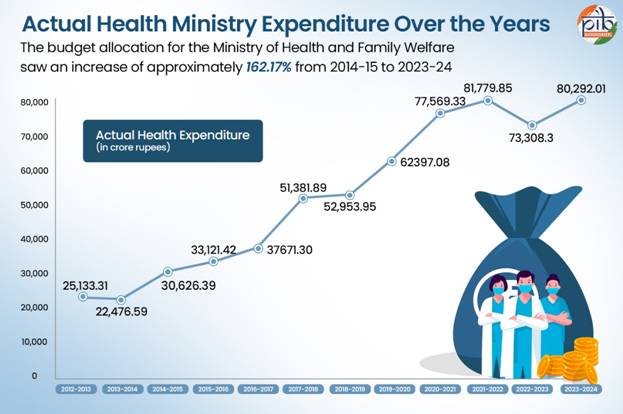
The Ministry of Health and Family Welfare has been allocated ₹1,06,530.42 crore in the Union Budget 2026–27, marking a 10 percent increase over the revised estimates of FY 2025–26. More significantly, this represents a 194 percent rise in health expenditure over the past 12 years. In addition, the Department of Health Research has received ₹4,821.21 crore, reinforcing the importance of innovation and scientific inquiry in shaping India’s medical future.
This steady upward trajectory in public health spending is not merely an accounting exercise. It signals a strategic reorientation—one that places universal health coverage, infrastructure strengthening, preventive care, digital health integration, and workforce expansion at the heart of national planning.
A Decade of Expanding Health Investment
The increased allocation for 2026–27 continues a decade-long pattern of rising public investment in healthcare. In contrast to earlier periods when health expenditure was often reactive and crisis-driven, recent budgets demonstrate a more structured and anticipatory approach.
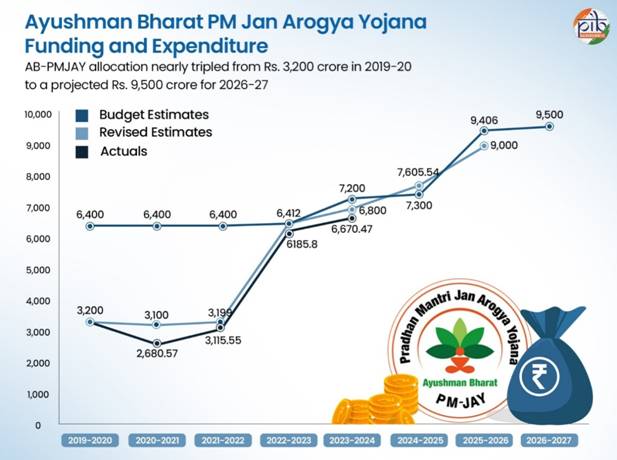
The Ayushman Bharat Pradhan Mantri-Jan Arogya Yojana (AB-PMJAY), launched in 2018, remains the world’s largest publicly funded health insurance scheme. With a budgetary allocation of ₹9,500 crore for 2026–27—up from ₹9,000 crore in the previous year—the scheme continues to provide health insurance coverage of up to ₹5 lakh per eligible household annually. It now serves over 12 crore vulnerable families, protecting them from catastrophic medical expenditure.
Similarly, the National Health Mission (NHM), which underpins primary healthcare services across rural and urban India, has seen its allocation rise to ₹39,390 crore from ₹37,100.07 crore. This increase reflects ongoing investments in maternal health, child immunisation, communicable disease control, and grassroots health infrastructure.
The Pradhan Mantri Swasthya Suraksha Yojana (PMSSY), aimed at correcting regional imbalances in tertiary healthcare, has received ₹11,307 crore, strengthening the expansion of AIIMS institutions and upgrading government medical colleges.
Particularly notable are sharp increases in certain targeted programmes. The National AIDS and STD Control Programme has witnessed a 30.64 percent rise in funding, while Blood Transfusion Services saw a 37.50 percent increase. These increments indicate renewed attention to public health surveillance, safe blood availability, and infectious disease management even as the country grapples with emerging non-communicable challenges.
The PM-Ayushman Bharat Health Infrastructure Mission (PM-ABHIM) has recorded one of the largest proportional increases—67.66 percent—underscoring the government’s focus on strengthening health systems capacity, including critical care blocks, integrated disease surveillance labs, and public health units at district levels.
Even institutional allocations reflect growth. AIIMS New Delhi, Central Government Health Scheme services, central hospitals, PGIMER Chandigarh, and the Indian Council of Medical Research (ICMR) have all received enhanced funding. The ICMR’s allocation, rising by nearly 27 percent, reinforces the importance of domestic medical research and biotechnology innovation.
Addressing India’s Epidemiological Transition
India’s health landscape has undergone a profound transformation. The Economic Survey 2025–26 highlights an epidemiological shift: while progress in maternal and child health has been remarkable—life expectancy has risen from 49.7 years in 1973 to 70.3 years in 2023—the burden of non-communicable diseases (NCDs) has surged.
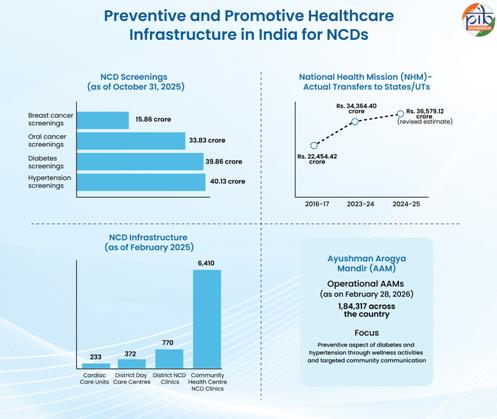
Cardiovascular diseases, diabetes, cancers, obesity, and chronic respiratory conditions now account for 57 percent of deaths in India between 2021 and 2023. These diseases are not confined to urban populations; they increasingly affect rural communities as well.
Recognising this shift, the government continues to strengthen the National Programme for Prevention and Control of Non-Communicable Diseases. Screening for hypertension, diabetes, and common cancers has been expanded through Health and Wellness Centres under Ayushman Bharat. Early detection, lifestyle awareness campaigns, and systematic referral mechanisms aim to reduce long-term treatment costs and mortality.
The Budget’s decision to grant 100 percent customs duty exemption on 17 new cancer drugs represents a direct intervention to reduce treatment costs for patients. By lowering import duties, the government seeks to ease financial burdens on families battling life-threatening illnesses.
Preventive healthcare, therefore, is no longer a secondary objective; it has become central to policy thinking.
Strengthening the Healthcare Workforce
Infrastructure without skilled personnel cannot deliver outcomes. Recognising India’s demographic profile—with a young population and growing elderly cohort—the Budget 2026–27 targets the training of 100,000 allied health professionals and 1.5 lakh caregivers over the next five years.
This initiative addresses two simultaneous needs: filling domestic workforce gaps and positioning India as a global healthcare talent provider. Allied health professionals—laboratory technicians, radiographers, physiotherapists, emergency responders—form the backbone of modern healthcare systems. Expanding this workforce will reduce patient load burdens and improve service delivery.
The proposal to establish a second NIMHANS-like institution in North India further signals the prioritisation of mental health. With rising stress, anxiety, substance abuse, and depression—particularly among youth—mental health services must expand beyond metropolitan centres.
Digital Health and System Integration
The Ayushman Bharat Digital Mission, allocated ₹350 crore, represents another crucial dimension of reform. Digital health IDs, electronic health records, and interoperable platforms are gradually transforming healthcare delivery into a more transparent and efficient system.
Digital integration reduces duplication of diagnostic tests, ensures continuity of care, and enables data-driven policy planning. In a country as vast as India, digital architecture is indispensable for achieving universal health coverage.
Infrastructure Expansion: Beyond Metro Cities
Healthcare inequity has historically been linked to geography. Tertiary care facilities were concentrated in urban centres, leaving rural and aspirational districts underserved.
Through PMSSY and PM-ABHIM, the government continues to expand AIIMS institutions and upgrade district hospitals. Investments in critical care blocks, disease surveillance networks, and emergency response systems are strengthening preparedness for future pandemics or health emergencies.
The expansion of medical colleges also contributes to both workforce supply and regional healthcare accessibility.
AYUSH: From Tradition to Global Leadership
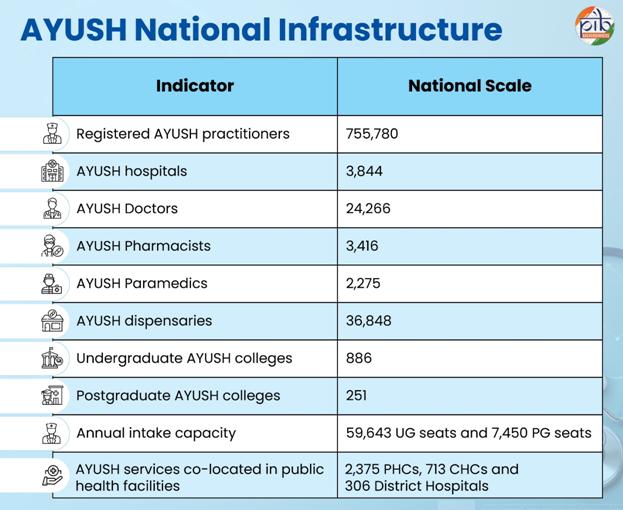
Perhaps one of the most distinctive features of Budget 2026–27 is the strategic positioning of AYUSH—Ayurveda, Yoga, Unani, Siddha, and Homoeopathy—as a modern, globally relevant healthcare system.
Post-COVID, preventive healthcare has gained renewed global attention. Ayurveda and holistic wellness systems have witnessed increased acceptance internationally. The Budget proposes establishing three new All India Institutes of Ayurveda and upgrading the WHO Global Traditional Medicine Centre in Jamnagar.
This move reflects more than cultural pride; it is an economic and diplomatic strategy. By strengthening research, education, and regulatory frameworks, India aims to position AYUSH as an evidence-based global health discipline.
Integration of AYUSH centres into regional medical hubs also enhances India’s medical value tourism. International patients increasingly seek integrative treatments combining modern diagnostics with traditional therapies. By embedding AYUSH into structured health ecosystems, India strengthens both its soft power and export potential.
Furthermore, AYUSH development supports rural livelihoods. Cultivation of medicinal plants benefits farmers, while processing and manufacturing create employment opportunities for youth.
Research and Innovation: Investing in the Future
The allocation of ₹4,000 crore to ICMR and ₹4,821.21 crore to the Department of Health Research underscores the importance of indigenous research capacity. From vaccine development to genomic studies and biotechnology startups, India’s healthcare future depends on sustained scientific investment.
The pandemic demonstrated the value of domestic research infrastructure. Strengthening it ensures preparedness against emerging pathogens, antimicrobial resistance, and future health crises.
Social Equity and Financial Protection
Healthcare reform cannot succeed without financial protection mechanisms. Rising medical expenses push millions into poverty annually. By expanding AB-PMJAY and strengthening CGHS services for pensioners, the government aims to reduce out-of-pocket expenditure.
Blood transfusion services, AIDS control programmes, and central hospital upgrades ensure that vulnerable populations receive targeted support.
Universal health coverage is not merely about hospital construction; it is about equity—ensuring that the poorest citizen has access to dignified care.
Healthcare as an Economic Multiplier
Healthcare investment generates broader economic dividends. A healthier population is more productive, innovative, and resilient. Reduced disease burden translates into higher labour participation and lower productivity losses.
Training allied health professionals and caregivers creates employment. Expanding biopharma research stimulates industry. Promoting AYUSH strengthens exports and tourism. Thus, healthcare becomes both a social obligation and an economic engine.
Toward Viksit Bharat 2047
India’s aspiration to become a developed nation by 2047 demands more than GDP growth. It requires a healthy, skilled, and secure population.
The Union Budget 2026–27 positions healthcare at the centre of this transformation. By combining increased funding, preventive focus, digital integration, workforce expansion, infrastructure development, research investment, and global AYUSH integration, the government has articulated a comprehensive roadmap.
Challenges remain. NCD prevalence is rising. Rural-urban disparities persist. Mental health stigma continues. Yet the direction is clear: healthcare is no longer reactive; it is strategic.
If sustained with accountability, transparency, and cooperative federalism, these investments can reshape India’s health landscape over the next two decades.
A Viksit Bharat in 2047 will not be measured solely by economic milestones but by the strength of its public health systems—by whether every citizen, regardless of geography or income, has access to quality care.
The Union Budget 2026–27 signals that India understands this fundamental truth: a developed nation must first be a healthy nation.






Comments are closed.